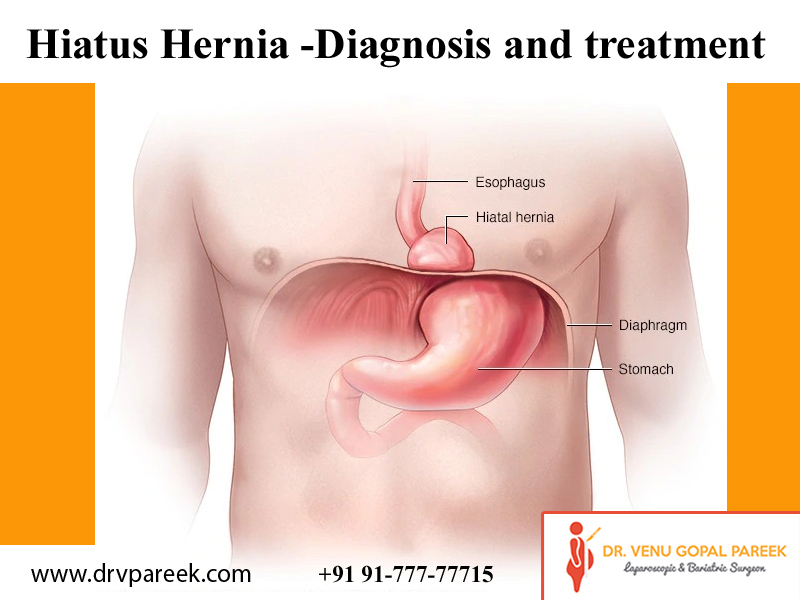
A hernia is a condition whenever the body’s inside is pushed into an area that doesn’t belong to it. A hiatal hernia occurs when the upper stomach is pushed through a small opening (hiatus) in the diaphragm and chest cavity.
The diaphragm is a large flat muscle that separates the lungs from the abdomen and helps us breathe. Not everyone with a hiatal hernia will experience symptoms. However, if you have a hiatal hernia, you are more prone to developing acid reflux in your oesophagus, which can cause heartburn and other symptoms. If symptoms do appear, treatment with acid-suppressing drugs usually works well.
Before exploring the many treatment options for Hiatal hernias, it is essential to understand the most common causes, risk factors, and symptoms associated with them.
What is a hiatal hernia?
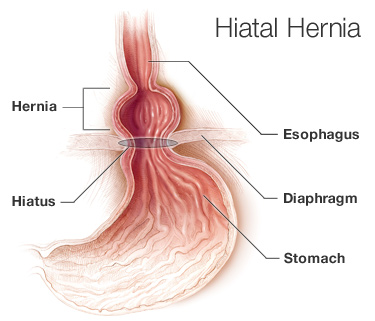
Food enters the mouth and then into the stomach via a pathway called the oesophagus. The diaphragm is a vital organ that helps with breathing and is located between the lungs and the stomach. The oesophagus flows through an opening in the diaphragm called the oesophagal hiatus.
A hiatal hernia is a condition in which the upper part of the stomach, which is just below the diaphragm, exits through the oesophagus’s hiatus and rests against the chest. Other hernias can occur in the abdomen, thighs, navel, or groin, but the tissue that protrudes from this type of hernia is in the stomach.
Hiatal hernias can be very painful because the diaphragm muscle continuously squeezes stomach . To treat a hiatal hernia, we need to address the hernia causes, namely inflammation of the intestines and pH imbalance.
Type of hiatal hernia
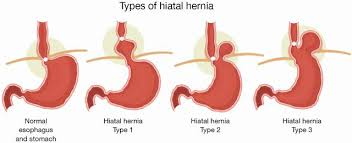
Sliding hiatal hernia is the most common type. The stomach enters at the oesophagus hiatus into the chest through an opening in the diaphragm. This muscle is what separates the lungs from the abdomen. The hernia can slide up and down on the lower chest, which is usually relatively small. This type of hiatal hernia is likely to be associated with acid reflux symptoms.
Paraesophageal hiatal hernia (also called rolling hiatal hernia) is less common. In this situation, the stomach is pushed down the oesophagus (protrudes) through the diaphragm’s opening. In some cases, other abdominal organs can also protrude through the opening. This can be the pancreas, spleen, or upper intestine (small intestine). This is not a standard type of hiatal hernia and is much less common than a sliding hiatal hernia. It is riskier because the protruding organs may jam and cause a blockage.
What are the symptoms of a hiatal hernia?
Many people with a small hiatal hernia have no symptoms and may never realize they have the condition unless it is accidentally discovered while investigating another problem. When symptoms appear, the most common symptoms are similar to those caused by gastroesophageal reflux:-
The symptoms are:
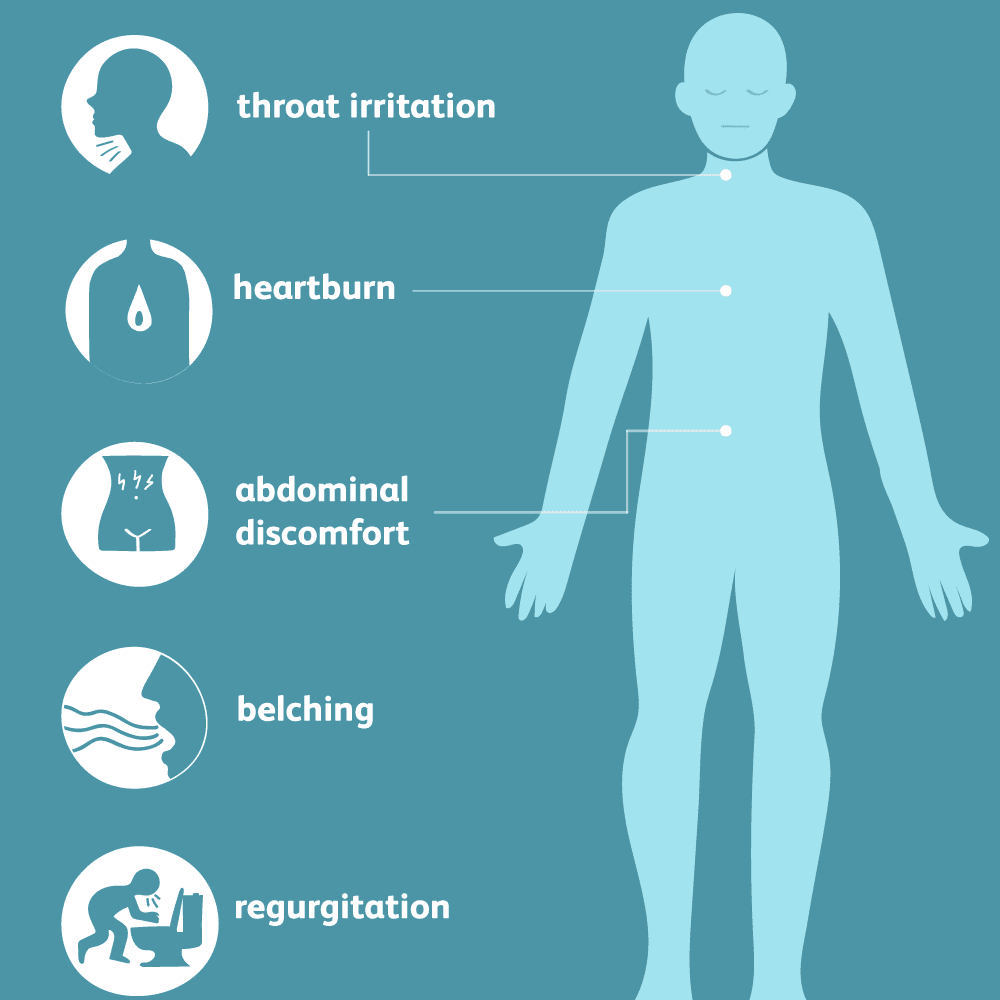
- Heartburn – a painful burning sensation in the lower front of the chest, behind the sternum and upper abdomen, often after eating or lying down.
- Burping of a sour or bitter-tasting liquid in the mouth, especially at night, along with severe reflux.
These symptoms often worsen when you bend over, lie down, or try hard to lift heavy objects. Depending on the type of hiatal hernia, other symptoms may include:
- Burping
- Difficulty in swallowing
- Pain when swallowing (hot drinks).
What causes a hiatal hernia?
The most common cause of Hiatal hernias is increased pressure in the abdominal cavity. This cavity includes the lower oesophagus, stomach, small intestine, large intestine, rectum, liver, gallbladder, pancreas, spleen, kidneys, and bladder. Pressure can come from many sources: coughing, vomiting, straining during bowel movements, weight lifting, exercise, pregnancy, obesity or excess fluid in the stomach. Other causes of a hiatal hernia include:
- Injury to the abdomen
- Diaphragm changes in adults
- Born with a very long hiatus.
Who is at risk?
While Hiatal hernias can develop in people of all ages and sexes, they are more common in people over 50, smokers, and overweight people.
How is a hiatal hernia diagnosed?
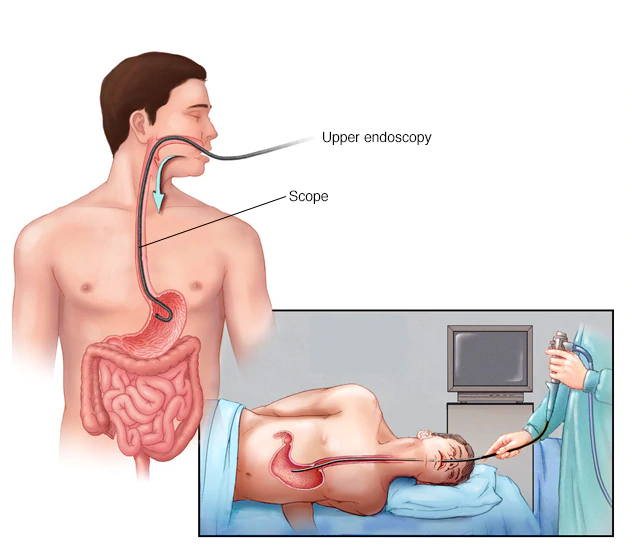
To diagnose a hiatal hernia, several tests can be done. This includes a barium take-up test, endoscopic procedures, oesophagal manometry test, pH test, and gastric emptying test.
- A barium test involves drinking a special liquid, and then an X-ray is taken to check for problems in the oesophagus and the stomach. It also shows how large the hiatal hernia is and whether the hernia is causing abdominal twisting.
- Endoscopy is a procedure that examines the inside of the upper digestive tract with an endoscope (a long, thin, flexible instrument about 1 cm in diameter).
- Oesophagal manometry measures the strength and coordination of the oesophagal muscles when swallowing.
- A pH test measures acidity in the oesophagus and helps determine symptoms related to acidity in the oesophagus.
- Stomach emptying studies look at how quickly food leaves the stomach. The results of this test are significant in patients with nausea and vomiting. Apart from Hiatal hernias, other causes of nausea and vomiting can occur.
Treatment of Hiatal hernias
Treatment for a hiatal hernia is usually only needed if it is causing problems. In most cases, people with Hiatal hernias will only have issues if the hernia causes gastroesophageal reflux disease (GERD). GERD can cause symptoms such as heartburn and a bad taste in the mouth.
Lifestyle changes and medication are the preferred treatments, although surgery can be used as an alternative to long-term treatment or when other treatments are not sufficient.
Lifestyle changes
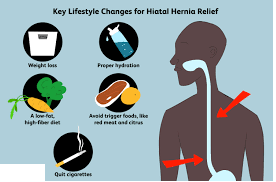
You can do several things on your own to help relieve the symptoms caused by a hiatal hernia. They include:
- Eat smaller meals, eat more often, not three large meals a day.
- Avoid lying down (including sleeping) for at least three hours after eating or drinking.
- Avoid drinking at night.
- Eliminate certain foods from your diet if you think they worsen your symptoms
- Avoid alcohol, caffeine, chocolate, tomatoes, fatty foods, spicy foods, and acidic foods or drinks such as lemon juice if they make your symptoms worse.
- Avoid slouching, especially after eating or drinking.
- Raise the head of your bed about 8 inches by placing a piece of wood or block under it. Don’t use extra pillows as they can put pressure on your stomach.
- If you are overweight, losing weight can help reduce the severity and frequency of symptoms.
- If you smoke, you should try to quit. Tobacco smoke can irritate your digestive system and worsen your symptoms.
Non-surgical treatment:

Since many hiatal hernia patients experience GERD symptoms, initial treatment is often started with GERD treatment. Your doctor may recommend a combination of lifestyle changes and medications that include:
- Antacids to neutralize stomach acid (i.e. Tumi, Rolaids)
- Medicines to reduce acid production known as H-2 receptor blockers (i.e.Pepcid, Zantac, Tagamet)
- Acid inhibitors – proton pump inhibitors that allow healing of the oesophagus (i.e. Prevacid, Prilosec)
Surgical treatment
Surgery is usually recommended for Hiatal hernias when the problem is not responsive to lifestyle changes and medication. You may also consider surgery if you have persistent and bothersome symptoms but don’t want to take medication for a long time.
How is hiatal hernia surgery performed?
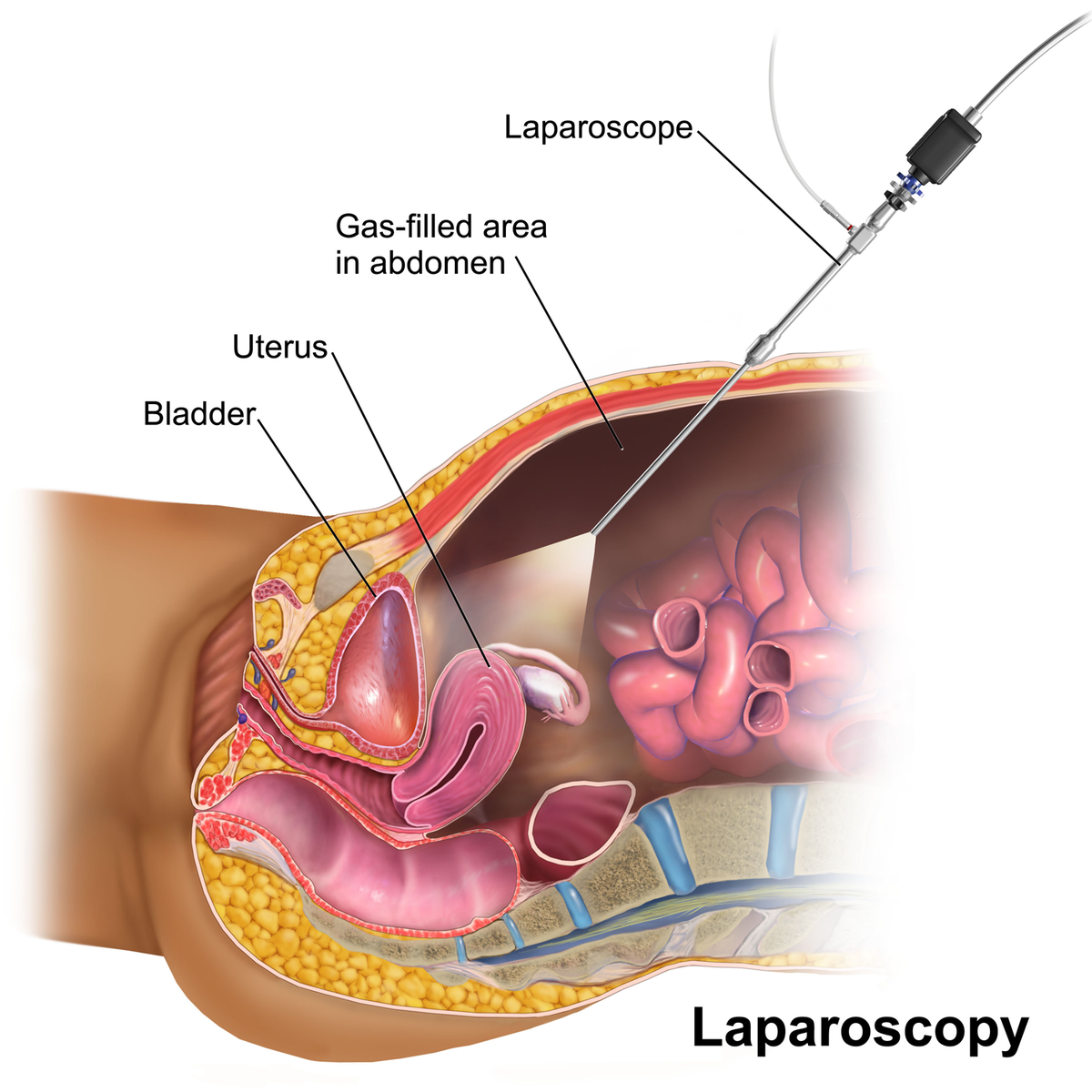
Hiatal hernia repair includes:
- Pull the hiatal hernia back into your stomach.
- Restoration of the valve at the bottom of the oesophagus.
- Closing the opening in the diaphragm muscle.
During surgery, your surgeon wraps the upper part of the stomach (called the fundus) around the lower part of the oesophagus. This creates a permanently tight sphincter (valve) muscle so that the contents of the stomach don’t return (reflux) into the oesophagus.
Surgery is called fundoplication, and there are two versions of this operation:-
Open fundoplication surgery involves a larger incision. This procedure may be required in some very severe cases and allows for better visibility during surgery. However, open surgery requires a longer hospital recovery time. In most cases, surgeons choose the laparoscopic approach.
Laparoscopic surgery is performed through the use of several small incisions instead of one large incision. This is considered a minimally invasive option. The specific laparoscopic procedure used to repair a hiatal hernia is called a Nissen fundoplication. This procedure creates a permanent solution for your hiatal hernia symptoms. During the procedure, your surgeon will make two or three small incisions in your abdomen. A laparoscope (a device that allows the surgical team to view your internal organs on a screen in the operating room) and other surgical instruments are inserted through small incisions. The fundus encloses the oesophagus, and the sphincter contracts during surgery. The advantages of laparoscopic surgery over open surgery include:
- Smaller incisions.
- Less risk of infection.
- Less pain and scarring.
- A shorter recovery.
Conclusion:
You may need to take medication for pain or may need to change your diet. However, one may require long-term treatment if the underlying disease is more severe. In some cases, they may need surgery to treat hiatal hernia.
Once your doctor has diagnosed the cause, he or she can develop a treatment plan to relieve the symptoms. Changing the food you eat can help treat acid reflux, which is caused by a hiatal hernia. If you are having trouble identifying the triggers, keep a food journal. Don’t live in discomfort. Contact Dr Venu Gopal Pareek if you have concerns about a hiatal hernia. Always remember that if your symptoms change or they get worse, you should see your doctor. Contact Dr Venu Gopal Pareek on 091777 77715 and book your appointment.