Thyroid removal is a standard surgical procedure that involves removing the thyroid gland. Previously, thyroidectomy was performed as an open procedure with an incision in the front of the neck that was usually longer than 6 centimetres.
Now surgeons use advanced techniques to operate on the thyroid. This operation is done through a tiny incision that is made at some distance from the gland. The surgeon does the operation with the help of an endoscope.
Your surgeon will discuss what options are available to you based on your needs, the surgeon’s experience, and the hospital’s equipment. Not everyone qualifies for a minimally invasive approach.
Let us see this article provided by Dr Venu Gopal Pareek gives information about Minimally invasive thyroid surgery.
What is Minimally Invasive Thyroid Surgery
Minimally invasive thyroid surgery is mainly determined by reducing the incision’s length to minimize postoperative pain and shortening hospital stay length. However, the most important thing is to improve the overall cosmetic result. This minimally invasive technique has been introduced over the past 15 years, with the sole aim of treating surgical thyroid disease with minimal pain, complications and aesthetics.
The thyroid is located in the neck area, below the larynx (voice box or “Adam’s apple”) and above the collarbone (collarbone). Surgery in this area for the glandular disease can produce large, noticeable scars after surgery.
There are currently two approaches to minimally invasive thyroid surgery:
- Minimally invasive open thyroidectomy (MIT)
- Minimally invasive video-assisted thyroidectomy (MIVAT).
Minimally invasive open thyroidectomy (MIT)
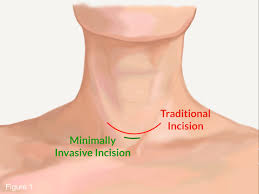
Overall MIT is similar to conventional open thyroidectomy. The main difference is the length of the incision in the neck, which must be less than 3 cm (1 inch) to be considered minimally invasive. Smaller incisions result in better overall cosmetic satisfaction and less patient discomfort. Apart from the incisions’ size, there are no other technical differences between MIT and traditional open thyroid surgery.
Minimally invasive video-assisted thyroidectomy (MIVAT)
MIVAT usually has an incision no more than 3 cm (1 inch) and is placed slightly higher than the traditional thyroidectomy incision in the neck. After the incisions are made, the surgeon uses an endoscopic video-assisted technique to insert a tiny camera into the incision and use it to visualize the surgical field. With advances in fibre optics and surgery, surgeons have performed significant surgeries without making large open incisions. This method also results in minimal blood loss and usually a faster operation speed, so that the patient is not exposed to anaesthesia.
Dr Venu Gopal Pareek determines whether he will use MIT or MIVAT or the combined approach during surgery by seeing patients conditions. He had experience performing several thousand of these procedures.
Surgical anatomy
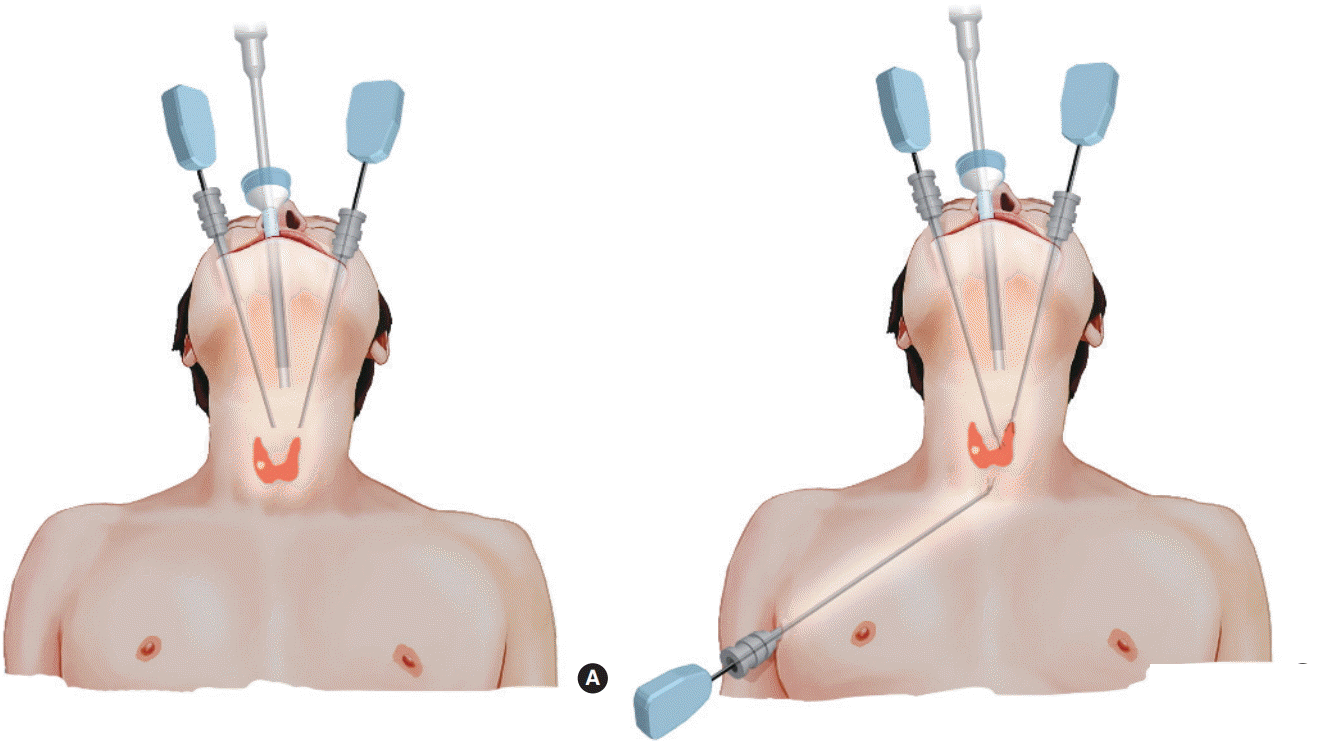
The thyroid is located in the neck’s midline, the thyroid is butterfly-shaped, about two inches high, and consists of two parts (i.e. like butterfly wings). There are also four small parathyroid glands in the thyroid, which play an essential role in our body’s calcium balance. During thyroid surgery, doctors preserve the parathyroid glands. The thyroid gland receives a dual blood supply, with one artery supplying blood to the top of the gland and the other artery supplying blood to the bottom.
An essential component of this anatomy is recurrent left, and right laryngeal nerves, whose injury to these nerves presents an obvious risk for thyroid surgery. The right recurrent laryngeal nerve is more susceptible to injury, but bilateral nerve damage can also occur. Due to the nerve’s closeness to the thyroid gland, doctors look at the larynx during thyroid surgery to prevent nerve damage. Nerves are responsible for motor function and feeling of the larynx (“voice box”). Therefore, injury to this nerve can cause hoarseness, disturbed voice list, loss of voice, difficulty swallowing or breathing.
Who is eligible for minimally invasive thyroid surgery?
One of the problems with minimally invasive thyroid surgery is that not all patients are eligible for this procedure. In general, patients are considered suitable for minimally invasive thyroid surgery if they have small thyroid nodules, thyroid volume is less than 20ml (this is usually determined by ultrasound) if they have not had previous throat surgery or therapy or neck radiation if the patient does not have thyroiditis. Patients with malignancy are usually treated with open thyroidectomy. Patients best suited for minimally invasive thyroid surgery have small nodules located in the regular or slightly enlarged thyroid gland.
The results of minimally invasive thyroid surgery
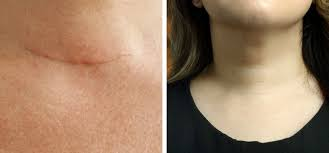
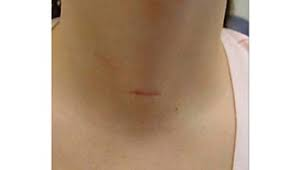
Open thyroidectomy is a safe procedure with few complications and yields good results for patients. The main problem with open procedures is that sometimes the patient is dissatisfied with the appearance of scars. Minimally invasive thyroid surgery was developed to reduce the size of the neck scar. The minimally invasive thyroid surgery results in carefully selected patients are promising candidates suitable for minimally invasive surgery. Sometimes chosen patients for minimally invasive surgery are not eligible for this procedure (usually because their thyroid gland is too large) are converted to open procedures for the best results.
Patients undergoing minimally invasive surgery are usually observed at night in the hospital for any complications. This is also the standard for many patients undergoing open procedures. The rates of complications, including postoperative bleeding, recurrent laryngeal paralysis, and hypocalcemia after minimally invasive thyroid, are comparable to open procedures. The minimally invasive technique can be associated with better cosmetic results and less postoperative pain.
Conclusion:
MIVAT and MIT is a safe and effective procedure which is clearly described as “minimally invasive”. It seems that MIVAT will survive the era of innovative technology and thyroid scar surgery.
Minimally invasive thyroidectomy is a procedure that very few surgeons perform daily. The operation in a competent surgeon’s hands produces excellent results with minimal downtime and most thyroid nodules, hyperthyroidism, goitre, and thyroid cancer can be treated with minimally invasive thyroid surgery. Every week the patient flies around the country to see Dr Venu Gopal Pareek. Most patients arrive the day before surgery and fly or drive 24-48 hours after surgery. Contact Dr Venu Gopal Pareek for best treatment at 091777 77715, and He has highly trained nurses and staff, and he handles this operation 5-10 times a week.