The whole world is currently battling with a new virus called COVID-19 or Coronavirus 19. COVID-19 spreads rapidly from one person to the other and is transmitted through direct contact and surface contact. Amidst the COVID-19 pandemic, patients suffering from critical illnesses need emergency surgeries/procedures. Delaying these surgeries could be dangerous. As per the directives received from the Ministry of Home Affairs, and keeping in mind the damage COVID-19 virus could do, all non-emergency surgeries must be postponed. Dr Venu Gopal Pareek and his surgical team are in strict adherence with these directives. However, if it is a case that warrants immediate surgical intervention, special consideration is being given.
As was established earlier, COVID-19 spreads through human-to-human transmission. It is transmitted mainly through aerosol from coughing, sneezing, or exhaling. Covid-19 is also transmitted when a person comes into direct contact with an infected person or through surface contact and then touching mouth, nose, or eyes. The high-risk individuals, of contracting the COVID-19, are those who have close contact with suspected/confirmed COVID-19 patients.
This article provides information about minimizing the risk of COVID-19 infection during emergency surgeries. These guidelines apply to healthcare professionals and others working in hospitals, laboratories, and primary health service centres. As a medical organization, we take adequate precautions in safeguarding the health and well-being of our health workers and staff in the operating room.
Use of Personal Protective Equipment (PPE):

The use of Personal Protective Equipment (PPE) is of the utmost importance when performing any emergency surgical procedure on patients when COVID-19 spread is at large. Personal Protective Equipment comprises all the protective covers designed to ensure the health of individuals by minimizing exposure to biological agents.
PPE, which is suitable for various types of patient interactions, must be made available. It must include personal clothing to shield medical personnel from contaminated blood, saliva or other potentially infectious material (OPIM).
PPE Components:
PPE includes safety goggles, face shields, masks, gloves, overalls/dresses (with or without an apron), headcover and outer shoes. Each component and the reason for its use is described below:
Face shield and goggles:
Contamination of the mucous membrane of the eyes, nose, and mouth from droplets brought about by coughing or sneezing of an infected person during a surgical procedure is likely to release aerosols into the air. Another possibility is touching of eyes, nose, or mouth with hands which have come in contact with the contaminated area. Hence, shielding of the mucous membranes of the eye, nose, and mouth with a face shield ensures safety. Safety glasses/goggles with broad frames cover a good layer of facial skin, eyes and the surrounding area.
Mask:
Coronavirus targets the upper and lower respiratory tract predominantly. Therefore, shielding the airways from droplets/aerosols prevents infections. This virus can also enter the host if the mucous membranes of the mouth and nose are contaminated by infectious droplets or by contaminated hands; hence masks come into play. They shield the nose and mouth from microorganisms. There are two types of masks recommended for healthcare professionals depending on the work environment:
- Three-layer medical masks: Three-layer medical masks are fluid-resistant masks. The material used in these masks protects the wearer from infectious material released while coughing, sneezing or talking.
- Respiratory masks (N-95): N-95 class of masks are respiratory protective devices with a high filtration efficiency. They are airtight but allow easy inhalation and exhalation, and provide a close facial fit to the wearer. When used properly, the filtering capacity of this mask is far superior to that of the three-layer medical mask. As these masks offer air seals, they are much tighter than three-layer medical masks.
Gloves:
If we touch an object/surface that has come in contact with a COVID-19 infected person and then touch our eyes, nose, or mouth, there is a huge chance of the virus making a way into our body. Care must be exercised when handling objects/surfaces that may be contaminated by suspected/confirmed COVID-19 cases.
Nitrile gloves are preferred over latex gloves because they can withstand chemicals including some disinfectants such as chlorine. Also, persons allergic to latex would prefer nitrile gloves to avoid allergic reactions such as dermatitis. However, if there are no nitrile gloves, latex gloves can be used. Non-abrasive gloves must be used over powdered gloves.
Coverall/Gowns:

These protect the upper body from exposure to the virus. Overalls provide 360-degree protection covering the entire body, including the lower back, legs, and sometimes the head also. An apron can also be worn above the overalls when the doctor is in the operating room. Overalls’ manufacturing complies to strict standards which prevent exposure to biological contaminants.
Shoe covers:
Shoe covers must be made of waterproof material so that the shoes are safe from contamination and dampness.
Headcover:
Headcover usually covers the head. Those who wear gowns must use head cover, which includes the head and neck while providing clinical care to patients. Hair and hair extensions must be pushed inside the headcover.
Anaesthesia precautions:
Anaesthesia is crucial for any surgical procedure and is of three types, namely:
- Local: This type of anaesthesia helps stop the sense of pain in a small area of the body that needs treatment. E.g., in a fingertip wound, local anaesthesia is given to clean the wound and dress it up.
- Regional: Regional anaesthesia is helpful in numbing pain in a rather large area of the body. E.g., in a large open wound of the leg or hand, anaesthesia is given to clean the wound and for operating.
- General: General anaesthesia renders the whole body unconscious, usually used in performing significant operations.
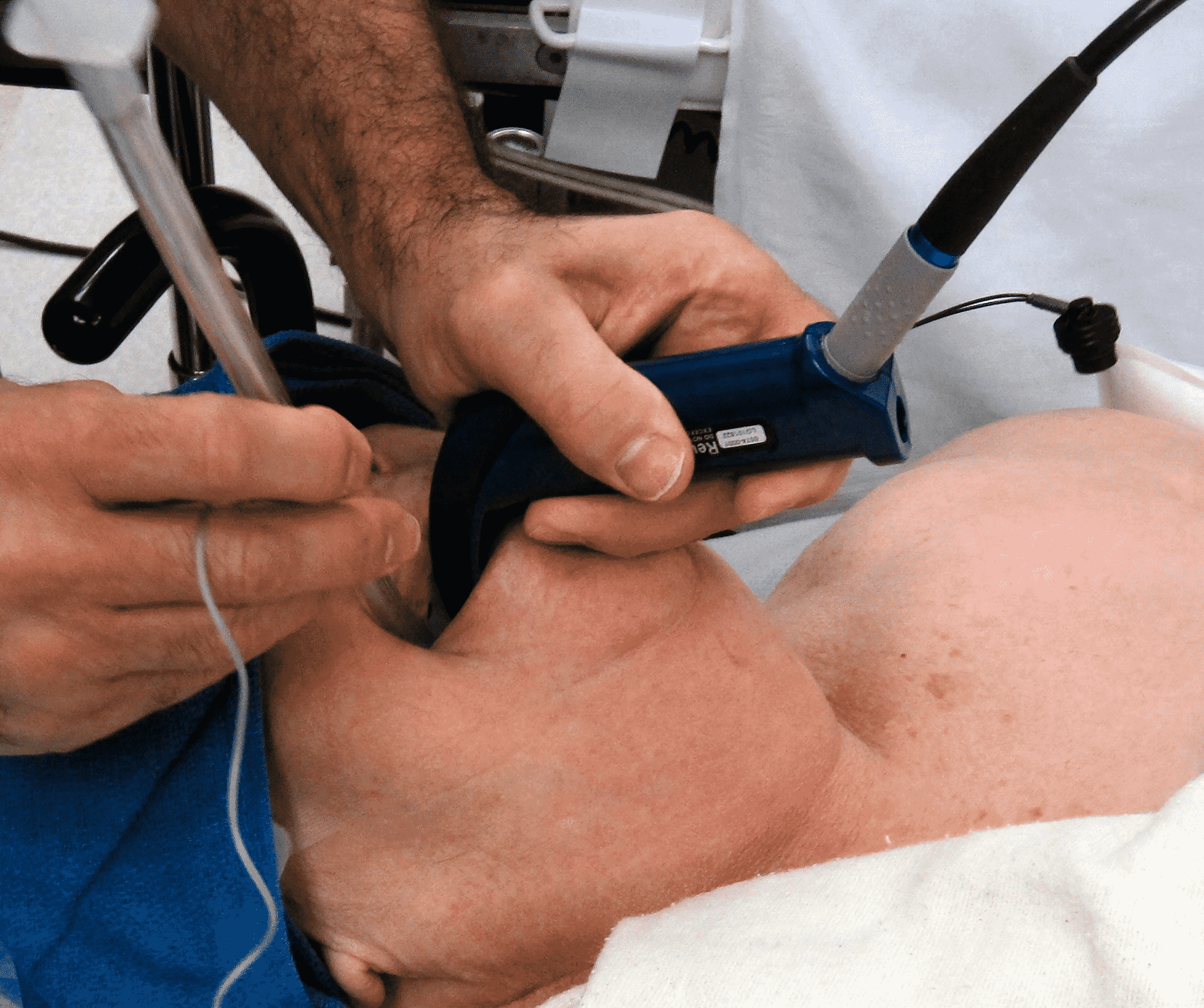
Anaesthesia is given via an injection, a breathing mask, or given through an intravenous line. In general anaesthesia, the patient cannot breathe on his/her own and needs a ventilator. This process involves placing a pipe (endotracheal) through the mouth into the airway.
The risk of aerosolization and droplets increases with procedures such as endotracheal intubation, tracheotomy, gastrointestinal endoscopy and during the evacuation of pneumoperitoneum and aspiration of bodily fluids during laparoscopic procedures.
Aerosolization (dispersal of fluids in the form of a fine spray) and droplet transmission of the COVID-19 virus are hazards for surgical personnel. Hence, procedures involving aerosolization should be avoided in the operating room. For example:
- High flow nasal cannula (more than 6 litres per minute)
- Nebulizers. Others might consider nebulizers as a non-aerosol process. We note it here because spraying can cause coughing.
- Awake fibreoptic intubation
- Entonox / inhalation sedation
- Non-invasive ventilation.
- Masking bag
- Use T-pieces or other open circuits
- Open suction.
Surgeons and staff not required for intubation must remain outside the operating room until anaesthesia. If general anaesthesia is needed, the surgical team must leave the room during intubation and extubation, except the surgical team (e.g. ENT / OMFS) directly involved in respiratory management. You can return in 15 minutes.
Standard surgery precautions:
Standard precautions for surgeries should focus on infection prevention practices that apply to all patient care, regardless of the patients’ infection status. These practices protect and prevent the spread of infection among patients and doctors. Standard precautions include:-
- Hand hygiene
- Use of personal protective equipment
- Respiratory hygiene/cough etiquette
- Sharps safety
- Safe injection practices
- Sterile instruments and devices
- Clean and disinfected environmental surfaces
Conclusion:
A careful planning of surgery procedure and adequate donning of PPE is very important and the most effective way to prevent exposure to the virus. Needless to say, and as is mentioned above, avoid non-emergency operations. Apart from the appropriate usage of PPE by the healthcare professionals, the clinical facility must have a stringent safety protocol in place and equipment for thorough sterilization of not just the hospital premises but also the surgical tools.
Dr Venu Gopal Pareek with his vast experience has a better understanding of the epidemiology, modes of transmission, and the methods to be followed for effective prevention. Dr Venu Gopal Pareek believes in the fact that a hygiene-conscious surgical team caters not only to the safety of the medical professionals and staff but also of the patients. This mantra does relate well to the environment created by COVID-19 virus. For more information in this regard, please contact Dr Venu Gopal Pareek at +91 91-777-77715.